HEALTH
Is red light therapy effective for rosacea? | A Review of the Evidence
Red light therapy is well-studied for things like wound healing, inflammation, collagen production, and various related skin conditions including rosacea. Acne rosacea is a common inflammatory skin condition affecting mainly the central face. Its typical manifestations are generalized erythema, telangiectasia, edema, papules, pustules, or a combination of all. In 2004, the National Rosacea Society (NRS) Expert Committee published a report on the classification and staging of rosacea that gives a definition of rosacea. Four subtypes of rosacea can be recognized on the basis of different morphological characteristics. It’s usually benign, but it can be quite frustrating for those who suffer from it. This blog will explore the available research on red light therapy for rosacea and make a decision about whether or not red light therapy is effective for the treatment of this skin condition.
What is rosacea? Symptoms and causes
Rosacea often starts with a tendency to flush and blush frequently. In time, persistent areas of redness appear on the cheeks and nose. The chin, forehead, and neck can also be affected. Tiny blood vessels may be visible. There may be inflamed, red bumps and pimples (papules and pustules) on the cheeks, chin, or forehead. The skin is often very sensitive and may feel dry, rough, or swollen.
Causes of rosacea:
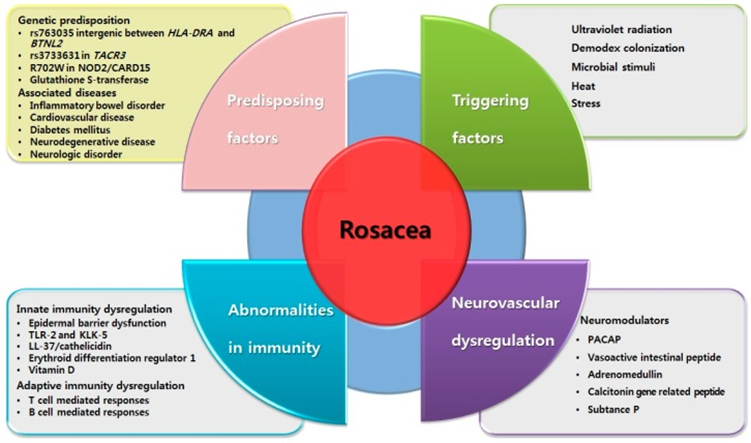
The exact pathology of rosacea is still unknown, but there are various reasons to trigger the breakout, such as an overactive immune system, heredity, environmental factors, or a combination of these. Second flare-ups might be triggered by hot drinks and spicy foods, alcoholic beverages, temperature extremes, the sun, emotions, exercise, drugs that dilate blood vessels, and cosmetic products.
The four subtypes of rosacea are recognized on the basis of different morphological features: erythematotelangiectatic, papulopustular, phymatous, and ocular. The erythematotelangiectatic subtype is the most common one, followed by papulopustular, phymatous, and ocular types, which are reported as less common. Clinical data showed that patients often harbor more than one rosacea subtype.
Clinical studies on the efficacy of red light therapy for rosacea
Red light therapy is a type of phototherapy that uses red LED lights to treat rosacea. Clinical studies have shown that this treatment is effective in reducing the symptoms of rosacea, and previous research has also reported the efficacy of red and blue lights for rosacea. Blue light (400–470 nm), due to its lower penetration, is useful in such skin conditions related to the epidermis layer of the skin, and thus it is able to interfere with human sebocytes proliferation, while red light (630 nm) is reported to have a significant effect on sebum production. Moreover, one study on rosacea-like mouse skin reported the efficacy of LED at 630 and 940 nm on the down-regulation of key inflammatory mediators in rosacea.
LED red light therapy interacts with the immune system
There is reported evidence of the efficacy of LED therapy in its interaction with the skin microbiome, and this could also have a significant impact on the etiopathogenesis of rosacea through immune response modulation. The microbial unbalance of the skin microbiota has been linked to rosacea clinical manifestations, even though the direct correlation is still under investigation. Authors reported the role of intestinal dysbiosis in promoting inflammation and impairment of normal lymphocyte function, potentially perpetuating chronic, low-grade inflammation. A higher incidence of small intestinal bacterial overgrowth was observed when patients with rosacea were compared to controls.
LED red light therapy interacts with sebum secretion
In comparison with blue light, the red light wavelengths penetrate more deeply into tissue, and it has been shown that red light can affect the sebum secretion of sebaceous glands and keratinocyte behaviors, as concluded in this study. The true function of these glands has yet to be investigated, but there are some proposed theories, including those regarding antioxidant effects, antibacterial effects, and the transport of pheromones. It is not unusual for the skin of a patient with rosacea to have increased or enlarged oil glands, which are called sebaceous hyperplasia. This glandular enlargement and oily skin seem to develop and progress unless the rosacea is treated.
LED red light therapy for inflammation
Red light also has anti-inflammatory properties through its influence on cytokine production by macrophages, as demonstrated in this experiment. Therapeutic approaches to rosacea focused on symptom suppression by means of anti-inflammatory agents such as doxycycline. Red light therapy can address inflammatory diseases as an alternative to conventional treatments. As one treatment that hits the core of rosacea symptoms, red light therapy dramatically helps reduce the appearance of facial redness, flushing, and telangiectasia.
Clinical cases for rosacea
There are some important references that verified the effectiveness of red light therapy for rosacea. In this study, there are two cases of clinical trials that used red light therapy to treat rosacea.
Case 1: A 22-year-old Caucasian woman with a 5-year history of pink eruptions on her nose. She was diagnosed as having papulopustular rosacea subtype, moderate grade. A combined and sequential plan of blue (480 nm ± 15 nm, 300 J/minute) and red
(650 ± 15 nm, 100 J/minute) LED therapy regimen was planned for 15 minutes per trial, twice a week for a total of ten sessions through a quasi-monochromatic 120 LED system. The improvement result is shown in the following picture.
Case 2: A 68-year-old Caucasian man presented with a 7-year history of papulopustular rosacea, moderate grade, was submitted to LED therapy twice a week for a total of ten sessions, through a LED system of blue (480 nm ± 15 nm, 300 J/minute) and red (650 ± 15 nm, 300 J/minute) with sequential irradiation for 15 minutes.
Lastly, in this study patients subjective to the photodynamic therapy of red light therapy alone observed that clinical inflammatory lesions disappeared completely in all patients after 24 weeks. The lesions were irradiated with 100 mW/cm2, 80-90 J/cm2, LED red light (635 ± 15 nm) over 15 min in each session with four sessions at 10-day intervals.
Why choose Bestqool red light therapy devices?
Red light therapy is a treatment that uses red and near-infrared light to treat various skin conditions. Research has shown that using red light therapy can reduce the appearance of rosacea symptoms in some people. There are different types of devices available, so it’s important to choose the one that is right for you.
Choose a true medical-grade light therapy device
Bestqool red light therapy devices are FDA-registered to ensure medical-grade treatment. A medical-grade red light therapy device should be qualified from the following points: 1) The highest safety standards in the medical field, 2) The medical effectiveness of irradiance and wavelengths output, and 3) Efficacy and efficiency for treatments. Bestqool products are able to provide the most effective narrow band of red (at 660 nm) and near-infrared (at 830 nm) wavelengths, with a high level of irradiance by our advanced LED technology. A high level of irradiance as high as 100 mW/cm^2 as the direct output determines the efficacy and efficiency of light therapy treatment. Using 10 minutes of Bestqool products is equal to using 20 minutes of others.
Blue light therapy for rosacea
Numerous studies use a combinational light to treat rosacea, which shows a better result than using red light therapy alone. Blue light therapy also has anti-bacterial and anti-inflammatory properties which can enhance the effect of red light therapy. Bestqool also provides light therapy masks with a combination of red, near-infrared, and blue lights for patients with facial rosacea symptoms. Consult with your physician before making the optimal choice for you.
Harper Harrison is a reporter for The Hear UP. Harper got an internship at the NPR and worked as a reporter and producer. harper has also worked as a reporter for the Medium. Harper covers health and science for The Hear UP.










